With a 35-year history in Colorado and in the Denver Metro Area, the Colorado Coalition for the Homeless (CCH) has been at the forefront of working collaboratively toward the resolution and prevention of homelessness, providing integrated health care, as well as supportive and vocational services. As the owner and operator of 2,000 units of permanent supportive and affordable housing, and the operator of a Federally Qualified Health Center system, CCH has worked to create lasting solutions for families, children, and individuals who are experiencing, or are at-risk of, homelessness throughout Colorado.
As the COVID-19 pandemic overwhelmed Denver’s public services and shelters, CCH leveraged its existing partnerships and organizational resources and systems to roll out an effective, collaborative, and innovative response to the pandemic. Its comprehensive approach to managing the outbreak—providing integrated health care coupled with locations for isolation/quarantine—has already proven to be a powerful model of care for a highly vulnerable population. More broadly, it has underscored the link between housing and health, a concept that is central to CCH’s mission and advocacy efforts.
We met with Cathy Alderman, vice president of communications and public policy, to discuss CCH’s multi-pronged approach to addressing homelessness during the pandemic: housing, health care, supportive services, and advocacy. The following conversation has been edited for brevity.
Can you describe the approach you and your partners in Denver have taken to address the needs of homeless individuals during COVID-19?
The first thing that became very clear is that the status of being homeless is absolutely incompatible with this public health crisis. Lack of housing means an inability to shelter in place and access hand-washing stations, both of which have proven challenging. Because of the congregate setting that shelters provide, physical distancing is not possible. This created a problem early on, so we joined shelter providers in their effort to de-densify existing shelters and to set up an auxiliary shelter to address these critical public health needs.
Next, we had to address how to screen people coming to the shelter. Though we lacked adequate testing supplies, we created a clinical triage process to provide screening and determine the best next step for each client. We are now partnering with our local public health department to do testing at all of the other shelters as well. We also had to adjust our screening strategies—something we continue to do—as we learn more about the virus, including that asymptomatic individuals can be contagious.
Once screened, people with no symptoms were housed in an auxiliary shelter (one for men and one for women) where they received a bed, three meals a day, laundry services, internet access, restrooms, and showers, as well as primary, mental, and behavioral health care. We currently have clinical staff on site in a “pop-up” clinic that we set up inside the shelter. We also have a testing tent just outside the building. Between the two auxiliary shelters, approximately 700 to 900 people are served each night.
Individuals who tested positive, were symptomatic, or high-risk, had to be separated from the rest of the shelter guests to prevent exposure and the spread of COVID-19. To do this, we contracted with a number of motels to provide the necessary space for isolation/quarantine. We have about 800 rooms and separated these sites into two categories, (1) Activated Respite Sites and (2) Protective Action Sites.
Activated respite sites provide isolation/quarantine with medical, behavioral health, and case management support for those with a confirmed or suspected COVID-19 case. While there is no set amount of time that individuals can stay in Activated Respite, the typical stay has been seven to 14 days.
Protective action sites are for those who are not symptomatic but are high-risk. For example, they may be over the age of 65, immunocompromised, diabetic, obese, asthmatic, or possess other respiratory illnesses. If they were to be infected, they would very likely require critical care or hospitalization. In addition to offering a safe environment where these individuals were less likely to be exposed, we provided medical and clinical support to help them manage whatever condition has made them high-risk.
We have case managers and provide medical and behavioral health services at various levels across the three different types of sites. We have a more concentrated presence on-site in our COVID-positive facilities in order to prevent the deterioration of guests’ health and ensure we can get those in need to the hospital as quickly as possible. Another newly added component of our health care services has been medication delivery across these new sites. So far, we’ve done 3,000 deliveries of medication to motels and hotels to serve our clients, many of whom require between three and eight prescription drugs a day to address multiple health conditions.
In addition to the shelter and services, we realized early on that we were going to have to create a way to store and deliver personal protective equipment, medical supplies, food, and clothing to all of the sites. We set up a centralized supply center in one of our existing buildings. This allowed us to take in large donations and provide food and supply delivery for those at the activated respite and protective actions sites, where most clients have small refrigerators and microwaves. It also allowed us to provide clothing—an essential need—because most of our clients come directly from the streets with little more than a backpack worth of belongings. Since CCH is not a shelter provider with these items readily on-hand, so building this capacity was critical to ensure each of the sites have what they need.
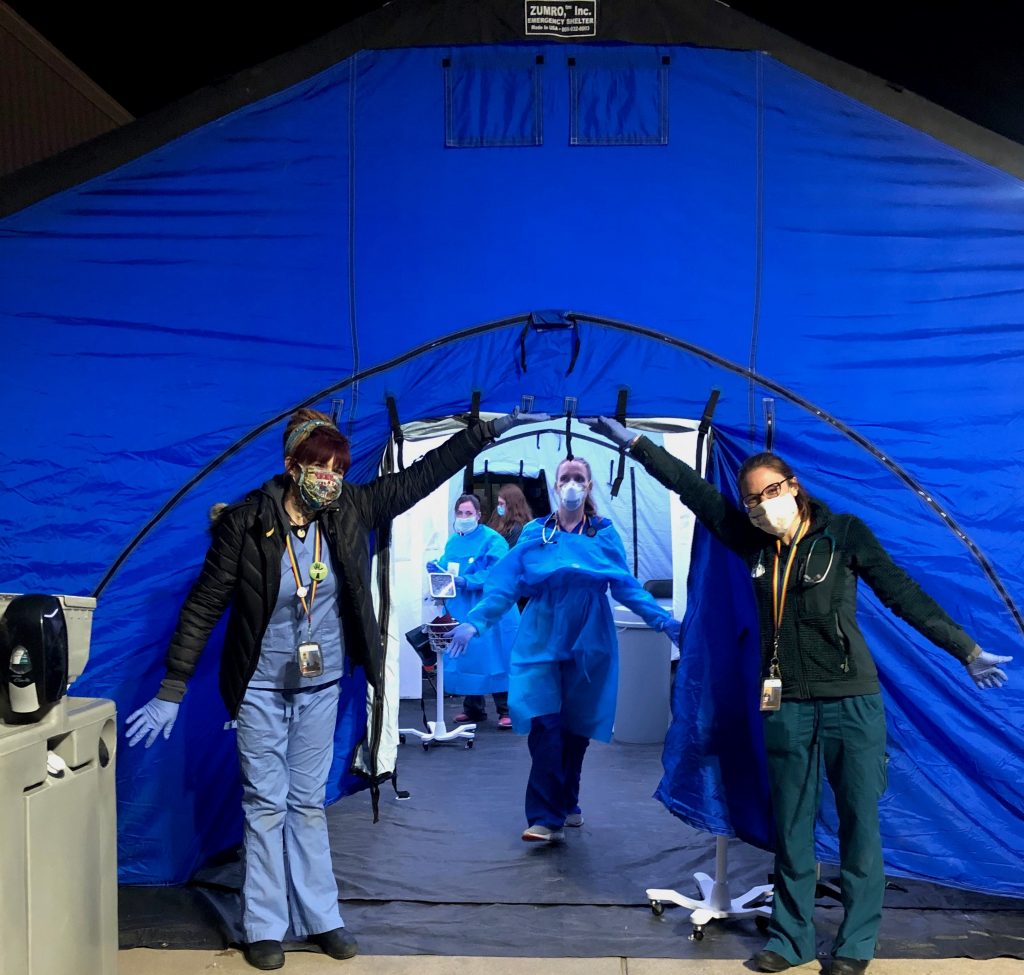
Can you tell us about ongoing testing efforts in Denver?
Now that testing supplies are more available, and our Denver Public Health (DPH) and Denver Department of Public Health and the Environment (DDPHE) have more staffing and supply capacity, we are expanding testing efforts. Originally, we were only able to test symptomatic individuals, primarily at our Stout Street Health Center. We are now able to do more widespread testing to isolate asymptomatic carriers and high-risk individuals. Our first testing pilot identified about a 20% prevalence rate of COVID-19 among asymptomatic individuals experiencing homelessness. We knew we needed to ramp up testing efforts quickly to identify and isolate those asymptomatic carriers so that they wouldn’t spread the virus to more high-risk individuals. DPH and DDPHE now have ongoing testing efforts at all of the shelters. We were also able to conduct a testing pilot for a small, unsheltered group who were camping in downtown Denver. Of the 50 people we tested, zero had positive results. This indicates to us that during this crisis response, we need to assist our unsheltered population with sanitation supplies, services, and access to housing, and not move them around the city where they are more likely to be exposed to the virus.
The Importance of Telehealth in the Time of COVID-19
CCH was using telehealth on a limited basis and also working on state legislation to better facilitate the provision of telehealth services. In response to COVID-19, they have greatly expanded their capacity so that their Federally Qualified Health Centers could continue to provide medical support and services.
- CCH purchased equipment to make sure clients had the resources they needed to utilize telehealth services during COVID-19.
- Colorado’s Medicaid agency implemented an emergency rule for the reimbursement of telehealth, which has been very helpful and allowed CCH to scale telehealth services.
- Building on the work done pre-COVID-19 and the lessons learned from this crisis, CCH is looking at legislative and regulatory actions that will better facilitate the provision of telehealth services.
- Going forward, CCH sees opportunities to expand telehealth to their properties. For example, sending a nurse with a computer to check in on residents and help them connect with a doctor via video as necessary.
How have your existing partnerships helped you respond to the needs of your clients during the pandemic?
The partnerships we have built over the years have been an invaluable resource for our COVID-19 response. Two years ago, we partnered with the shelter provider community across Denver to create the Homelessness Leadership Council (HLC). Through HLC, we have been able to provide collective and consistent feedback and strategy recommendations to the City for assisting our unhoused community. Our meetings over the last two years, and the trust and collective expertise we have built as a community, has been a great asset in delivering a comprehensive response to address the unique needs of our community during the pandemic.
Using hotel and motel rooms to meet COVID-19 needs seems like a unique solution. How did you come up with this approach?
Last year, we purchased a motel and spent six months converting it into 139 studio apartments called Fusion Studios. This required interior renovations to make the rooms code-compliant with full-time, residential property building standards. In February, we started moving people in. Prior to Fusion, we owned another motel that we used for bridge and transitional housing that we turned into permanent supportive and affordable housing. At the time, we didn’t realize we were going to have to ramp up to this level so quickly. We are always on the lookout for opportunities to convert hotels into housing.
For our COVID-19 response, we negotiated with each motel separately, addressing their particular issues and liability concerns, also taking into account the specific services being provided at each location. Given the emergency declaration, we have been able to use the Federal Emergency Management Agency (FEMA) to serve as reimbursement to acquire these spaces and to manage any damage that occurs on site. In addition, in some cases, we have the option to purchase their facilities after a period of time of use. We are constantly evaluating what the next stage of our COVID-19 response efforts will look like, and how long these spaces will be needed. We are considering purchasing two of the properties to provide housing for people who don’t need to be in the hospital, but need to isolate or recover and don’t have a home.
What do you think are the next steps after responding to the immediate crisis? Are there areas you would like to focus on more going forward?
First, we are actively thinking through a rehousing strategy, now that we are moving beyond the immediate crisis. After the pandemic is over, what do we do with the 800 clients we have in motel rooms, and the 700 to 900 individuals in our auxiliary shelters? Do we send clients back to the shelter or to the street? That is not an option, especially with those individuals we’ve removed from congregate settings because they’re high-risk. Instead of putting people back in high-risk environments, we need to find more transitional housing options. We’re working to find the resources to create more permanent supportive housing down the road, including converting more motels to meet these needs.
Second, in the aftermath of COVID-19, I can’t imagine a world where we don’t have a clinical component to our shelters. The lesson this pandemic taught us is that it’s imperative to couple shelter/housing with clinical services, and we and our shelter partners are looking to advance this model. Our shelter providers have been appreciative of the clinical staff on site, because that’s not their area of expertise. They serve in the role as emergency responders and while they can do non-clinical health screens, they are not equipped to manage ongoing or long term physical or behavioral health issues. I envision transitioning back to multiple shelter environments, each one with clinical services onsite, or with a clinical component employing our mobile health unit for regular site visits.
Cathy spoke on CCH’s work for NHC’s Solutions for Housing Communications convening in May 2020. You can view her presentation here. Learn more about CCH’s areas of expertise and response to COVID-19 here.